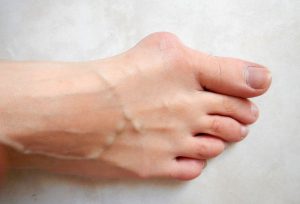
What is a Bunion?
A frequent cause of disability from foot pain is the bunion. A bunion typically appears as A bony bump that forms on the base of the big toe. They affect some 35% of women over the age of 65. If left untreated and allowed to progress to its eventual end stage, the deformity can impair your ability to perform every day activities like walking or stair climbing. At this end stage surgery is the recommended treatment solution to resolve the deformity. But get this – up to 15% of bunions return following surgery. The reason for this is simple. It is because the underlying muscle weaknesses that lead to your original bunion formation still remain. Weak muscles directly contribute to the formation of your bunion but strengthening those same muscles is also your cure. Before it gets too late try physical therapy and the exercises below to help resolve the impairments of this foot disorder.
How Your Physical Therapist Can Eliminate Bunion Pain
The three exercises below are a great place to start in your bunion recovery process. In addition to these self-help exercises, your Physical Therapist can eliminate bunion pain by assessing:
- Walking: This takes into considering not just your feet motion, but also abnormalities in the knee, hip and back that can decrease strain on the foot.
- Soft tissue problems: The bones and joints of the foot are supported by muscles and tendons. We place unnecessary stress on the foot and ankle muscles that Physical Therapists can identify.
- Footwear: This depends on the shape and arch support you may need for ideal foot loading. Your physical therapist can also guide you on proper shoe selection to improve your ability to walk and exercise without discomfort.
Final Directions
The exercises—foot scrunch, toe yoga, and heel raise—are easy to do at home and can strengthen these key foot muscles. Stronger feet may help decrease bunion-related pain and its impact on movement. Exercises are progressed from sitting, to standing on both feet, to performing the exercises standing on just 1 leg. Perform exercises daily for best results. For more information on nonsurgical options for treating bunions, contact your physical therapist specializing in orthopedic injuries.
Citation
Deschamps K, Birch I, Desloovere K, Matricali GA. The impact of hallux valgus on foot kinematics: a cross-sectional, comparative study. Gait Posture. 2010;32:102-106. http://dx.doi. org/10.1016/j.gaitpost.2010.03.017
Hurn SE, Vicenzino B, Smith MD. Functional impairments characterizing mild, moderate, and severe hallux valgus. Arthritis Care Res (Hoboken). 2015;67:80-88. http://dx.doi.org/10.1002/ acr.22380
Glasoe M, Ward. “Treatment of Progressive First Metatarsophalangeal Hallux Valgus Deformity: A Biomechanically Based Muscle-Strengthening Approach” (J Orthop Sports Phys Ther 2016;46(7):596- 605. doi:10.2519/jospt.2016.6704).
The information provided on this site is intended for your general knowledge only and is not a substitute for professional medical advice or treatment for specific medical conditions. You should not use this information to diagnose or treat a health problem or disease without consulting with Heather Lane Physical Therapy or another qualified healthcare provider.

