Osteoporosis (OP) screening is now on many doctors’ radar for patients as young as age 50, especially for those at high risk. Previously, osteoporosis would typically not be diagnosed until a fracture occurred. Today’s practice of earlier screening gives the patient a better chance of avoiding the worst effects of OP.
Do you have OP?
Affecting more than 200 million people around the world, OP is the most common bone disease in humans. People with OP have low bone density, low bone mass and changes in their bone structure.
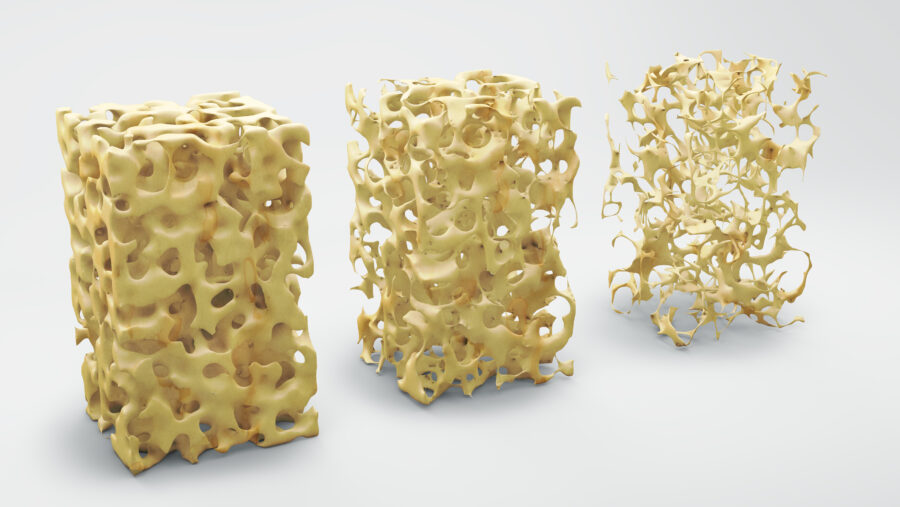
All of these changes cause bones to break more easily. Think of bones as having an internal structure like a honeycomb. People with osteoporosis have more space in their honeycombs than people who do not have the disease. The walls of their honeycombs are thinner, too.
Risk factors for developing osteoporosis include:
- Being female
- Being postmenopausal without taking estrogen
- Losing weight
- Smoking
A doctor who determines that you should be screened will order a bone density scan to compare your bone structure and density to a baseline of people with healthy bones. Your doctor will tell you whether the bone density scan indicates that you have osteoporosis.
Treatment options for OP
If you learn that you have OP or that you are at risk for it, your doctor may recommend that you take a drug or supplement.
- Medication. Several options are available. Your doctor will explain the differences in benefits and side effects.
- Estrogen supplement. Estrogen has been shown to promote bone growth, but studies show that estrogen also can cause headaches, nausea and an increased chance of some cancers.
- Calcium and vitamin D supplement. Calcium + vitamin D also has been shown to promote bone growth and halt bone loss. However, there is controversy over how much to take and how much this helps.
Physical therapy to stop OP progression
For a low-risk approach to stopping the progression of osteoporosis, doctors and patients turn to physical therapy. Targeted exercises help to preserve bone density, prevent bone cells from dying and keep bones strong.
But be careful! The wrong kinds of exercise can cause fractures in already weak bones. A physical therapist can plan your regimen so that the exercises are safe for you if you have osteoporosis or are at risk for developing it. Your PT will customize the treatment plan to your specific condition, make sure that bones that are already fractured or fragile will not be further stressed and watch you to check that you’re doing the exercises safely and effectively.
Citations
Hannan, M. T., Felson, D. T., Dawson-Hughes, B. , Tucker, K. L., Cupples, L. A., Wilson, P. W. and Kiel, D. P. (2000), Risk Factors for Longitudinal Bone Loss in Elderly Men and Women: The Framingham Osteoporosis Study. J Bone Miner Res, 15: 710-720. doi:10.1359/jbmr.2000.15.4.710
Kim, M. H., & Lee, H. J. (2016). Osteoporosis, vitamin C intake, and physical activity in Korean adults aged 50 years and over. Journal of physical therapy science, 28(3), 725–730.
doi:10.1589/jpts.28.725
Kunutsor, S. K., Leyland, S., Skelton, D. A., James, L., Cox, M., Gibbons, N., … Clark, E. M.
(2018). Adverse events and safety issues associated with physical activity and exercise for
adults with osteoporosis and osteopaenia: a systematic review of observational studies and an updated review of interventional studies. Journal of frailty, sarcopenia and falls, 3(4), 155-178. doi:10.22540/JFSF-03-155
Santos, L., Elliott-Sale, K. J., & Sale, C. (2017). Exercise and bone health across the lifespan. Biogerontology, 18(6), 931–946. doi:10.1007/s10522-017-9732-6
Sözen, T., Özisik, L., & Basaran, N. Ç. (2016). An overview and management of osteoporosis. European journal of rheumatology, 4(1), 46–56. doi:10.5152/eurjrheum.2016.048
Troy, K. L., Mancuso, M. E., Butler, T. A., & Johnson, J. E. (2018). Exercise early and often: effects of physical activity and exercise on women’s bone health. International journal of environmental research and public health, 15(5), 878; doi:/10.3390/ijerph15050878

